TOOTH CONTACT AREAS IN SLEEP AND AWAKE BRUXISM
Anastasia Slavicek1,2, Florian Slavicek2, Nicola Furlini3, Ksenia Nafigina4, Gregor Slavicek2
1Dental Clinic Smile-time, RU-142106 Podolsk, Moscow Region, Russian Federation
2Orehab Minds GmbH, DE-70567 Stuttgart, Germany
3Studio Furlini, IT-38122 Trento, Italy
4German Implantology Center, RU-121059 Moscow, Russian Federation
Abstract:
Introduction: Bruxing is one of the occlusal functions that has to be considered as potential risk factors for restorative and prosthetic rehabilitations. Visualizing and quantifying the extent of tooth grinding contributes to the decision-making process for both dentists and patients. Currently, little attention is paid to the distribution of grinding tooth contacts in the dental arches. The lateral and sagittal distribution of tooth contact areas supports the alertness for heavily loaded dental arch segments and those segments that are not or only slightly involved.
Patients and Method: Based on two case reports, the strongly varying distribution of tooth contact areas during bruxing, especially for the sleeping and waking states, can be can be analyzed easily, practicably and without risk for the patient. Both patients received two BruxCheckers, one to be used during sleep, the other one during work.
Results: The analysis of the BruxCheckers based on number and size of the tooth contact areas showed a similar result for one, but significantly different results for the other patient, comparing sleep and awake bruxism. The analysis of lateral and sagittal distribution based on number and size (mm2) gives detailed information about occlusal functional quality. The distribution of tooth contact areas can be identical in sleep and awake bruxism; but such an accordance should not be assumed in every case.
Conclusion: Knowing the actual involvement of occlusion during bruxing allows refining occlusal changes. TCAs‘ lateral and sagittal distribution provides deep insight into the unconscious occlusal function of tooth grinding and helps to realize those occlusal segments less involved in the bruxing pattern. An analogous result for sleep and awake Bruxing on the BruxChecker should not be taken for granted.
Introduction:
Dental practitioners are interested in the best possible care for their (bruxing) patients. As oral rehabilitation always includes irreversible occlusal changes, understanding the location and size of occlusal contact areas within the dental arch is crucial for establishing the therapeutic strategy. Understanding the potential risk of tooth grinding/clenching will help to modify a therapeutic strategy. Bruxism is possibly associated with prosthetic failures [1]. Expert opinions regarding the best therapeutic concepts of bruxism (awake and asleep) differ substantially. Instead of the term „therapy“ the phrase „management“ is often utilized [2].
Practicable screening tools for assessing tooth grinding activity prior to any occlusal intervention have low costs, easy to handle, no side effects, and an additional diagnostic benefit. The BruxChecker® (BC; Scheu Dental, DE-58642 Iserlohn, Germany) visualizes the contacts between teeth originating during unconscious teeth grinding or clenching during awake and asleep state. The BC is fabricated for the individual patient using the pressure molding technique. First, preliminary data have been published, allowing a numerical comparison of number and size of tooth contact areas (TACs) with norm values [3].
A paradigm shift in assessing SB has occurred in recent years. SB is no longer understood solely as a harmful movement disorder. However, most clinicians focus primarily on possible negative consequences of bruxism: chipping, occlusal trauma, tooth migration, temporo-mandibular disorder [4]. Different, quite controversial opinions on the significance of teeth grinding in humans in medicine and dentistry exist. Is it an abnormal function, a movement disorder [5]? Or, in contrast, can tooth clenching during bruxing be assessed as a relevant physiological occlusal function [6]? This view shows that parafunction represents a secondary function besides primary occlusal functions. The growing acceptance of considering bruxism (awake and asleep) as a physiologic function modifies the fundamental methodical approach. Today bruxism (awake and asleep) is graduated in possible (based on patient’s self-reports), probable (determined by clinical inspection), and definite (verified by an instrumental analysis) [7]. This classification is not an either/or choice. The international consensus group formulates a precise grading in favor of instrumental analysis. Tooth clenching and grinding may be assessed differently considering clinical consequences: harmless, with little clinical relevance; at least one negative consequence, such as chipping; or at least one positive consequence, including end of breathing suspension and increased salivation [7].
Preliminary data (young adults, males and females, natural occlusion with minimal restorations) will help to understand better occlusal involvement in bruxism. Based on these data, a quantitative and qualitative appraisal of individual patients is available in daily practice. The mean value of the number of TCAs is ≈28 (sd +/-8). The mean size of TCAs is ≈70mm2 (sd +/-51mm2). The comparison between females and males shows only minor, not significant differences for number and of TCAs: males, an average of ≈29 (sd +/-8) TCA´s with an average size of ≈87mm2(sd +/-58), while for females, ≈27 (sd + / -7) TCA´s with an average size of ≈56mm2 (sd +/-40mm2). Further attention during the analyses of BC has to be paid to the distribution of TCAs right and left, the transversal (lateral) distribution. The number of TCAs is almost identical on the right and left sides. There are only minor differences in the distribution of the size of TCAs on the right and left. The evaluation of the sagittal distribution considers three sections: anterior (corresponds largely to anterior teeth including the canine), intermediate (corresponds largely to the premolar region), and posterior (corresponds largely to the molar region). The sagittal distribution of TCAs in the upper jaw is ≈8 (sd +/-3) anterior, ≈7.5 (sd +/-2.5) intermediate, and ≈12.5 (sd +/-5) posterior. The following values describe the mean size of TCAs: for the upper occlusion ≈28mm2(sd +/-24mm2) anterior, ≈14mm2 (sd +/-11mm2) intermediate and 3≈0mm2 (sd +/-25mm2) posterior [3].
The BC visualizes functional TCAs. For this reason, the authors of this article suggest a different, systematic approach for the BC analysis based on numerical data in order to compare the awake and asleep bruxing. This report aims to demonstrate to quantitative and qualitative data of occlusal contacts areas comparison of BC used during sleep and used during work, based on two case presentations.
Participant and Method:
Based on two clinical cases, the importance of understanding the differences between bruxing and tooth grinding during sleep and in awake state is highlighted.
Patient 1: 30-year-old male with natural occlusion (all 32 teeth present) and minimal restorations; dental class I on both sides; upper dental arch with slight compression in the premolar area, slight anterior narrowing in the lower jaw, isolated gingival recessions, and occlusal abrasions on the casts. Main concern of the patient: temporomandibular joint noises in both temporomandibular joints during (wider) mouth opening. In addition, the patient reports gastrointestinal reflux, sensitive teeth, slight headache and tension in the neck/throat along with postural problem. The patient is aware of grinding and clenching of teeth and wants to prevent tooth destruction and deterioration of joint noises and headache.
Patient 2: 33-year-old female with natural occlusion (wisdom teeth absent) and minor occlusal restorations in the molar region; dental class I on both sides; narrow upper arch, crowding in the lower anterior arch; gingival recession and class V lesion in both arches, most evident in upper canines and premolars right and left. Main concern: gingival recessions and joint noises left TMJ. In addition, the patient reports gastritis, headache (bilateral temporal and occipital region, tension type headache, during night and also in the afternoon), tinnitus right side combined with a feeling of swelling and sometimes hearing impairment and neck spasm. The clinical muscle and joint examination (palpation) supports a tentative diagnose myofascial pain syndrome with TMJ involvement.
Both patients received two BC, along with the instructions to use one BC during sleep (one night), the other BC during work (full day). After the BC have been returned to the dental clinic, a digital analytic process was performed online, and the clinic received two reports with the results in tabular, graphical and verbal form, one for the clinic, one for the patient in an electronic format (pdf).
Results and Discussion:
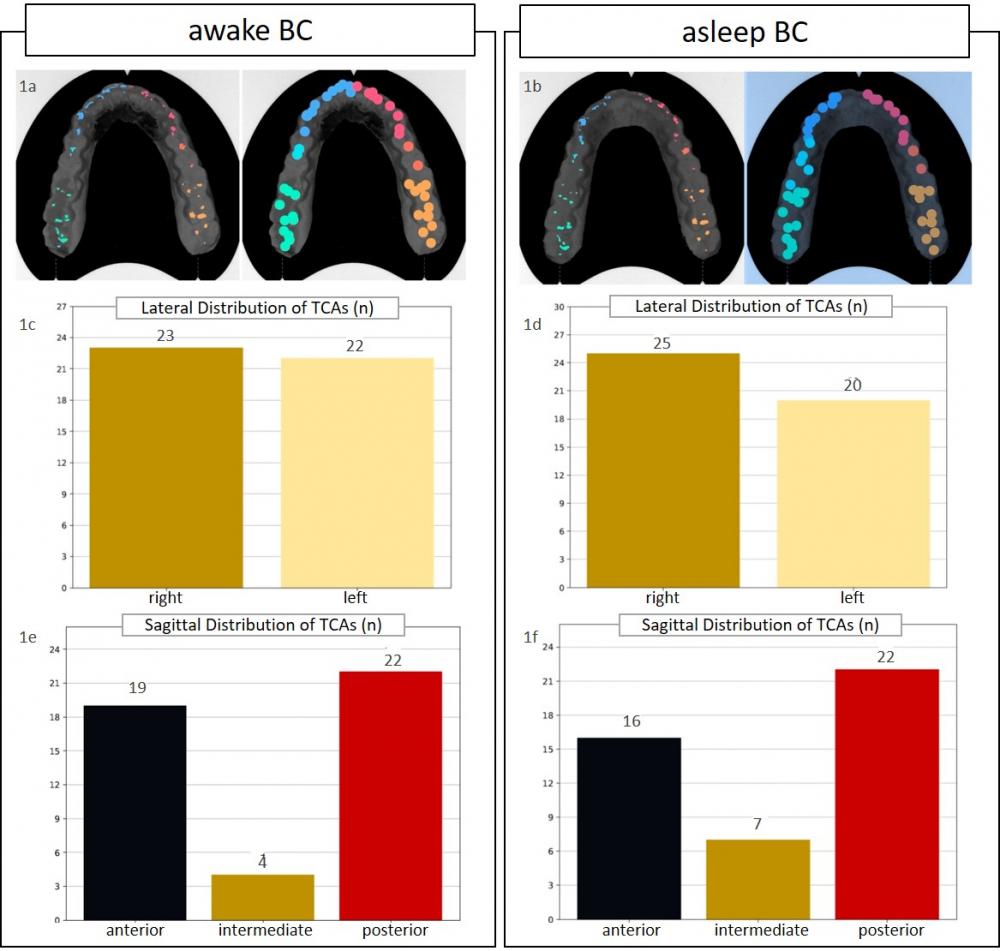
Results for Patient 1: The following comparison of the TCAs on sleep and awake BC show almost identical results in the lateral and sagittal distribution of the TCAs. (Fig. 1)
The lateral distribution of right versus left is very similar: awake BC with total 45 TCAs (61.7mm2), of which 23 (51.1%) TCAs (30.9mm2, 50.1%) are on the right side and 22 (48.9%) TCAs (30.8mm2, 49.9%) on the left side; asleep BC with total 45 TCAs (59.2mm2), of which 25 (55.6%) TCAs (29.4mm2, 49.6%) are on the right side and 20 (44.4%) TCAs (29.8mm2, 50.4%) on the left side. The sagittal distribution of anterior versus intermediate versus posterior reveals differences as well: awake BC anterior 19 (42.2%) TCAs (25.7mm2, 41.6%), intermediate 4 (8.9%) TCAs (6.7mm2, 10.8%) and posterior 22 (48.9%) TCAs (29.4mm2, 47.6%); asleep BC anterior 16 (35.6%) TCAs (20.8mm2, 35.2%), intermediate 7 (15.6%) TCAs (8.4mm2, 14.2%) and posterior 22 (48.9%) TCAs (30.0mm2, 50.7%).
The following comparison of the TCAs on sleep and awake BC demonstrate a significant difference, especially in the lateral distribution of the TCAs for patient 2. (Fig. 2)
The lateral distribution of right versus left shows significant differences for the awake BC with total 17 TCAs (32.1mm2), of which 6 (35.3%) TCAs with a size of 9.5mm2 (29.6%) are located on the right side and 11 (64.7%) TCAs with a size of 22.6mm2 (70.4%) are located on the left side. The lateral distribution for the asleep BC discloses significant differences: total 21 TCAs with a size of 36.9mm2, of which 14 (66.7%) TCAs with a size of 23.0mm2 (62.3%) are located on the right side and 7 (33.3%) TCAs with a size of 13.9mm2 (37.7%) are located on the left side. The sagittal distributions anterior versus intermediate versus posterior reveals for the BC used during sleep or in wake state are not so varying in the number of TCAs (awake BC anterior 7 (41.2%), intermediate 1 (5.9%), posterior 9 (52.9%); asleep BC anterior 7 (33.3%), intermediate 3 (14.3%), posterior 11 (52.4%). Significant differences are obvious in the size of the TCAs (awake BC anterior 5.3mm2 (16.6%), intermediate 0,2mm2(0.8%), posterior 26.5mm2 (82.6%); asleep BC anterior 21.0mm2 (56.8%), intermediate 4.2mm2 (11.5%), posterior 11.7mm2 (31.7%).
Occlusal rehabilitation aims to harmonize occlusion. This harmonization is traditionally seen from centric contacts and eccentric protrusive and laterotrusive guidance. Symmetric distribution of TCAs and a sagittal distribution following the accepted occlusal concepts (anterior control, posterior support, mutual protection) enables the clinician to establish objectives in occlusal function bruxism. Using the mean size of the TCAs for total, right, left, anterior, intermediate, and posterior helps estimate the distribution’s uniformity within the arch. Using such key figures will help to understand the occlusal asymmetry and disharmony. Table 1
Comparing the results of patient 1 with the preliminary standard values show, that the number of TCAs (45) is above average (28 +/-8) for both awake and asleep bruxism. The size of the TCAs (61.7mm2) is slightly lower than the average. The almost identical pattern of tooth contacts in sleep and in the waking state can also be represented by the mean size of all TCAs (table 1).
In contrast, the comparison of the results for patient 2 show a different outcome: the number of TCAs (17 awake BC, 21 asleep BC) are slightly reduced (28 +/-8). The size of the TCAs (32.1mm2 awake BC, 36.9mm2 asleep BC) is reduced, compared to the mean values. The very different pattern of tooth contacts in sleep and in the waking state can also be represented by the mean size of all TCAs, especially in the distribution (table 1).
Conclusion:
Knowing the actual involvement of occlusion during bruxing allows refining required occlusal changes. TCAs‘ lateral and sagittal distribution provides deep insight in the unconscious occlusal function of tooth grinding and helps to realize those occlusal segments less involved in the bruxing pattern.
The dental professionals may approximate the individual TCAs with the data on the number and size of the TCAs in natural occlusion to understand the amount of occlusal involvement of the individual patient. In addition, comparing the occlusal grinding pattern during sleep and awake state may modify the treatment details, such as the prescription pattern of intraoral splints (night, day, 24h). A similar result for sleep and awake Bruxing on the BruxChecker should not be taken for granted.
The visualization of the tooth grinding pattern helps the patient better understand the bruxing function. In addition, the comprehension of possible risk for the natural teeth and surrounding tissues and restorative materials raises.
In the authors‘ opinion, the quantitative approach to bruxing tooth contact areas will simplify the assessment of this occlusal unconscious function, both diagnostically and therapeutically. The author suggests, that additional to total number and size of tooth contact areas the lateral and sagittal distribution (qualitative analysis) has to be considered, and should not obscure the dental arch segments not involved in bruxing.
In the future, the quantitative and qualitative occlusal analysis will possibly allow a better understanding for the occlusal involvement in dysfunctional problem. Further research projects are required.
Conflict of Interest:
A.Slavicek (scientific advisor, lecturer), F.Slavicek (CEO) and G.Slavicek (owner, head R&D) declare a conflict of interest due to their involvement in the company Orehab Minds (Orehab Minds GmbH, DE-70567 Stuttgart, Germany; https://www.orehab-minds.com) that developed the automatic BruxChecker® analysis and now distribute it under the product name DRS BRUX.
- Chrcanovic BR, Kisch J, Larsson C, Analysis of technical complications and risk factors for failure of combined tooth‐implant‐supported fixed dental prostheses.“ Clinical implant dentistry and related research 2020; 22.4; 523-532 https://doi.org/10.1111/cid.12300
- Bussadori SK, Motta LJ, Horliana ACRT, et al. The Current Trend in Management of Bruxism and Chronic Pain: An Overview of Systematic Reviews. J Pain Res. 2020;13:2413-21 https://doi.org/10.2147/JPR.S268114
- Slavicek, G., Grimmer, D., Novitskaya, A., & Slavicek, F. (2021). On the track of bruxism: quantitative, qualitative and intraindividual analyses of the BruxChecker® in daily clinical routine. Stoma Edu J, 8(3), 163-171 DOI:https://doi.org/10.25241/stomaeduj.2020.8(3).art.2
- Onodera K, Kawagoe T, Sasaguri K, et al. The Use of a BC in the Evaluation of Different Grinding Patterns During Sleep Bruxism, CRANIO® 2006;24(4):292-9, https://doi.org/10.1179/crn.2006.045
- Sateia, MJ International classification of sleep disorders. Chest 2014;146.5:1387-94 https://doi.org/10.1378/chest.14-0970
- Slavicek R and Sato S „Bruxism–a function of the masticatory organ to cope with stress.“ [Bruxism–a function of the masticatory organ to cope with stress] Wiener Medizinische Wochenschrift 2004; 154.23;584-9 https://doi.org/10.1007/s10354-004-0129-1
- Lobbezoo F, Van der Zaag J, Van Selms MKA, et al. Principles for the management of bruxism. Journal of Oral Rehabilitation 2008;35(7);509-23 https://doi.org/10.1111/j.1365-2842.2008.01853.x
Legends:
Fig.1: Comparison of the two BruxChecker® (BC) of patient 1: 1a, 1c and 1e show the results for awake bruxism, 1b, 1d and 1f the results for bruxism during sleep; the transversal distributions are similar for awake and asleep grinding pattern
1a, 1b: highlighted tooth contact areas with allocation to occlusal segments and visualization of the size tooth contact areas, equal diameters of the circles indicate similar expansion of the tooth contact areas
1c, 1d: right and left distribution for number of TCAs
1e, 1f: distribution TCAs in sagittal direction – anterior vs. intermediate vs. posterior
Fig.2: Comparison of the two BruxChecker® (BC) of patient 2: 2a, 2c and 2e show the results for awake bruxism, 2b, 2d and 2f the results for bruxism during sleep; the transversal distributions are very different for awake and asleep grinding pattern
2a, 2b: highlighted tooth contact areas with allocation to occlusal segments and visualization of the size tooth contact areas, equal diameters of the circles indicate similar expansion of the tooth contact areas
2c, 2d: right and left distribution for number of TCAs
2e, 2f: distribution TCAs in sagittal direction – anterior vs. intermediate vs. posterior
Tab.1: quantitative analyses of the BruxChecker® for patient 1 and 2. Additionally, mean sizes of the TCAs are displayed (highlighted columns) – the significantly different values for patient 2 indicate that the distribution of the TCAs in the dental arch vary substantially. In addition, it can be recognized that teeth grinding is performed very differently during awake and asleep state.